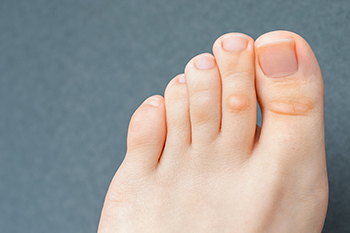
 Pain can often accompany a corn on the foot. A hard corn is defined as a small, toughened area that develops on top of the toes. It generally forms due to wearing shoes that do not fit correctly. The shoes may be too tight, and this can cause friction as the toes rub against the top of the shoes. A soft corn forms between the toes and is generally moist a majority of the time. Mild relief may be found when a protective covering is worn on top of the corn, or in between the toes. This can help to cushion and protect the corn as daily activities are completed. It is suggested to refrain from wearing high heels with an existing corn, in addition to limiting the amount of walking. If you have developed a corn, please speak to a podiatrist who can recommend proper removal techniques.
Pain can often accompany a corn on the foot. A hard corn is defined as a small, toughened area that develops on top of the toes. It generally forms due to wearing shoes that do not fit correctly. The shoes may be too tight, and this can cause friction as the toes rub against the top of the shoes. A soft corn forms between the toes and is generally moist a majority of the time. Mild relief may be found when a protective covering is worn on top of the corn, or in between the toes. This can help to cushion and protect the corn as daily activities are completed. It is suggested to refrain from wearing high heels with an existing corn, in addition to limiting the amount of walking. If you have developed a corn, please speak to a podiatrist who can recommend proper removal techniques.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact David Jenson, DPM, FAENS of Jenson Foot and Ankle Specialist. Our doctor will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in The Woodlands, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
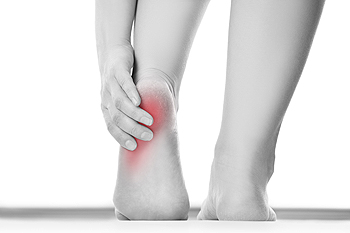
Read more about Understanding Corns and CallusesIf you have heel pain, you may have come across the medical term plantar fascia. This is a strong, fairly inflexible connective tissue on the bottom of the foot that connects the heel bone with the toes. When this tissue becomes damaged or torn, it is known as plantar fasciitis, a painful inflammation of the plantar fascia. There is a good chance that your heel pain may be caused by plantar fasciitis, as this is the most common form of heel pain. What caused your plantar fasciitis? Perhaps you run or walk quite a bit or have the type of job that requires you to stand for all or most of the day. Maybe you regularly wear flip-flops, high heels or other footwear that does not offer adequate support or cushioning. Arthritis can contribute to the development of plantar fasciitis, as well as tight calf muscles, high arches, flat feet, or other conditions you may have that cause an imbalance in the biomechanics of your feet. You may even be pregnant or carrying some extra weight, which can stress the plantar fascia. Whatever the reason is for your heel pain, you should know that help is available. You don’t need to learn to live with heel pain, especially if it is caused by plantar fasciitis. Podiatrists treat people with plantar fasciitis every day, and can offer you various forms of treatment to provide the relief you are looking for.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact David Jenson, DPM, FAENS from Jenson Foot and Ankle Specialist. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in The Woodlands, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Plantar Fasciitis
If you have cold feet on a regular basis, there may be a variety of causes. Sometimes, your feet are cold simply because of the temperature. Cold weather makes the blood vessels in the extremities constrict to help keep your vital organs warm. The same effect can be caused by high anxiety or stress. By far the most common cause of chronic cold feet is poor circulation. Lifestyle choices, such as being sedentary, sitting at a desk all day, or smoking often inhibit blood flow to your feet. Additional factors, such as high cholesterol, which works to restrict the arterial flow of blood, can result in poor circulation. Other causes include diabetes, anemia, nerve disorders and hypothyroidism. Anyone who experiences cold feet regularly would be wise to visit with a podiatrist who can diagnose their condition and prescribe proper treatment options. In the meantime, you can put on warm socks and slippers, take foot baths regularly, and take short walks to help get the blood flowing.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact David Jenson, DPM, FAENS of Jenson Foot and Ankle Specialist. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
- Muscle pain, stiffness, or weakness
- Numbness or cramping in the legs
- Skin discoloration
- Slower nail & hair growth
- Erectile dysfunction
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact our office located in The Woodlands, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Causes, Symptoms, and Treatment of Poor Blood Circulation in the Feet